| ⚠️ SEVERE ALLERGIC REACTION HAPPENING NOW?
If you or someone with you has trouble breathing, throat swelling, lightheadedness, vomiting, or sudden full-body hives — this may be anaphylaxis. 1. Use an EpiPen (epinephrine auto-injector) immediately if available — into the outer thigh. 2. Call 911 — even if symptoms improve after the EpiPen, you still need emergency care. 3. ER of Watauga is open 24/7 — call (817) 945-5500 |
An allergic reaction can range from a mildly itchy rash to a life-threatening emergency that unfolds in minutes. Knowing the difference — and acting fast — can save a life.
If you need allergic reaction emergency care in Watauga, TX, ER of Watauga provides 24/7 emergency treatment for everything from severe hives and asthma triggered by allergens to full anaphylaxis. Our board-certified emergency physicians, on-site lab, and IV-capable rooms allow us to stabilize and treat allergic reactions immediately — no waiting room, no transfer required.
This guide walks you through what an allergic reaction is, how to recognize the danger signs, when to use an EpiPen, when to call 911, and exactly how we treat allergic emergencies at our ER.
What Is an Allergic Reaction?
An allergic reaction is your immune system overreacting to a normally harmless substance — called an allergen. Your body releases chemicals (most importantly histamine) that cause symptoms ranging from minor itching to dangerous breathing problems.
Allergic reactions are categorized by severity:
- Mild reaction — local symptoms like a rash, mild itching, or runny nose. Usually manageable at home with antihistamines.
- Moderate reaction — symptoms spread beyond the exposure site (widespread hives, facial swelling, stomach upset). May need urgent medical care.
- Severe reaction — multiple body systems affected (skin + breathing + GI + cardiovascular). Requires immediate emergency care.
- Anaphylaxis — the most severe form. Rapid, full-body reaction that can cause airway swelling, dangerously low blood pressure, and death within minutes if untreated. Always a 911 emergency.
The same allergen can cause different severity levels at different times — meaning a person who once had only hives could have anaphylaxis on the next exposure. Past reaction severity is not a reliable predictor.
Common Allergens and Triggers
Allergic reactions can be triggered by almost anything, but some causes are far more common than others. The most frequent triggers we see in the ER include:
- Foods — peanuts, tree nuts, shellfish, fish, eggs, milk, soy, wheat, sesame
- Insect stings — bees, wasps, hornets, yellow jackets, fire ants
- Medications — penicillin and other antibiotics, NSAIDs, anesthetics, contrast dye
- Latex — gloves, balloons, certain medical equipment
- Environmental allergens — pollen, mold, pet dander, dust mites (typically cause milder reactions)
- Exercise-induced — rare reactions triggered by physical activity, sometimes combined with food
- Unknown triggers — about 20% of severe allergic reactions have no identifiable cause at the moment of presentation
If you have a known allergy, carry an EpiPen and your medical history with you at all times — and make sure family, friends, and coworkers know how to use it.
Allergic Reaction Symptoms by Severity
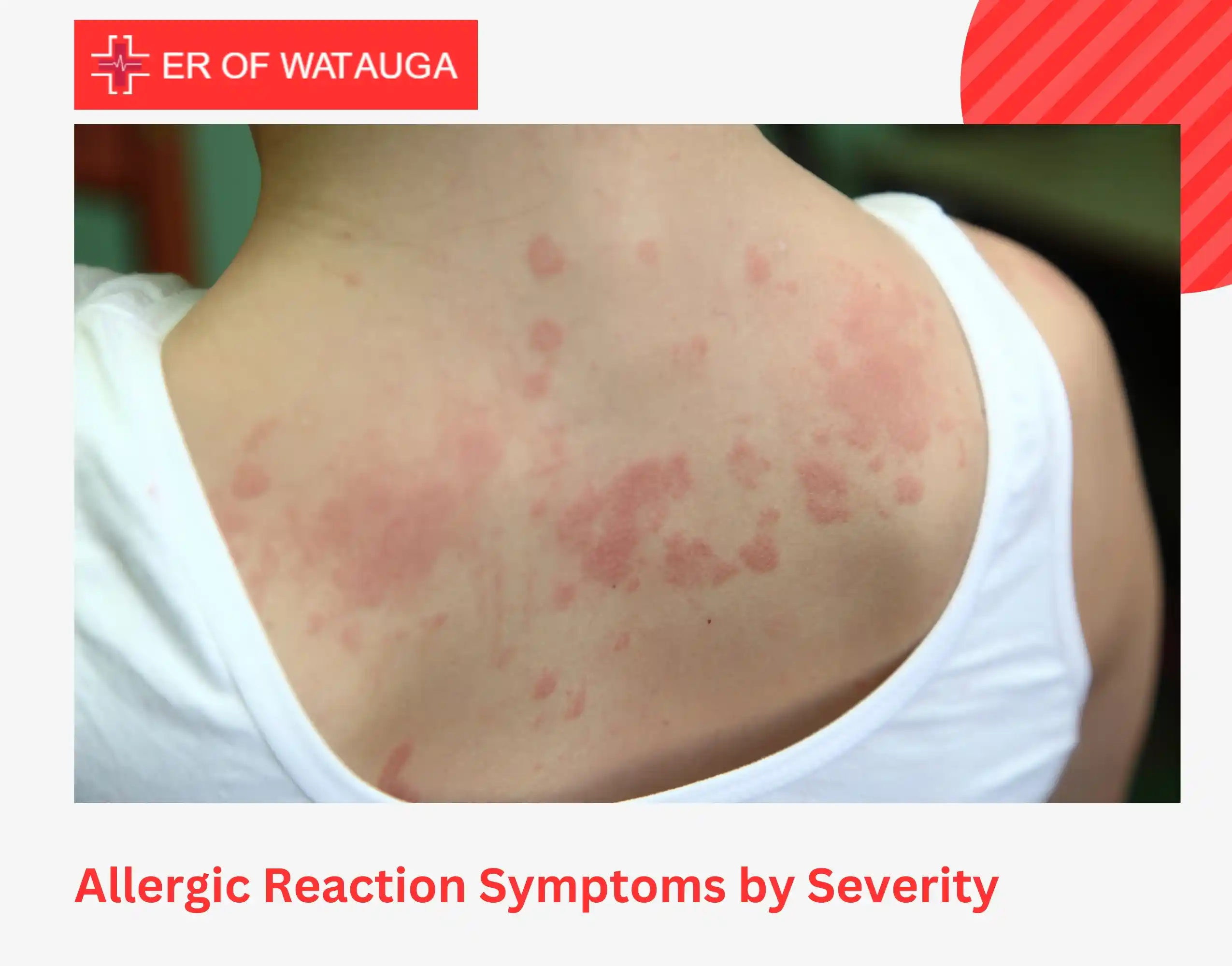
Symptoms typically appear within minutes to two hours after exposure. The faster symptoms develop, the more serious the reaction is likely to be.
Mild Symptoms
- Localized hives, itching, or a small rash
- Sneezing, runny nose, or mild congestion
- Watery, itchy eyes
- Mild stomach discomfort
- Slight tingling around the mouth (with food allergies)
Moderate Symptoms
- Widespread hives across the body
- Swelling of the face, lips, or tongue (angioedema)
- Persistent vomiting or diarrhea
- Wheezing or a tight feeling in the chest
- Significant stomach pain or cramping
Severe Symptoms (Possible Anaphylaxis — Call 911)
- Difficulty breathing or swallowing
- Throat tightness, hoarseness, or swelling
- Rapid or weak pulse
- Sudden drop in blood pressure (dizziness, fainting)
- Confusion or loss of consciousness
- Pale or bluish skin, lips, or nail beds
- Sense of impending doom
- Symptoms in two or more body systems happening together
Severe symptoms — especially when more than one body system is involved — should be treated as anaphylaxis until proven otherwise.
Anaphylaxis: A Time-Sensitive Emergency
Anaphylaxis is the most dangerous form of allergic reaction. It can progress from mild symptoms to airway closure or cardiac arrest in as little as 10 to 15 minutes — sometimes faster.
How to Recognize Anaphylaxis
Suspect anaphylaxis when any of the following happens after exposure to a likely allergen:
- Skin or mucosal symptoms (hives, swelling, itching) PLUS breathing difficulty OR low blood pressure
- Two or more of: skin symptoms, breathing problems, low blood pressure, or persistent GI symptoms
- Sudden drop in blood pressure after exposure to a known allergen — even without skin symptoms
How to Use an EpiPen
Epinephrine is the only first-line treatment that reverses anaphylaxis. Antihistamines and inhalers do not stop a severe reaction — only epinephrine does.
Step-by-step EpiPen use:
- Remove the EpiPen from its case
- Pull off the safety cap (usually blue)
- Hold it in your fist with the orange tip pointing down
- Firmly press the orange tip against the outer thigh — through clothing if needed
- Hold for 3 seconds while the medication delivers
- Massage the injection site for 10 seconds
- Call 911 immediately and bring the used EpiPen with you to the ER
Important: even if symptoms improve after the EpiPen, go to the ER. Anaphylaxis can return in a delayed second wave called a biphasic reaction — sometimes hours later — and a single EpiPen dose may not be enough.
When to Call 911 vs. When to Go Directly to the ER
Call 911 Immediately If:
- There is any difficulty breathing or swallowing
- The throat feels tight, scratchy, or swollen
- The person is dizzy, lightheaded, or losing consciousness
- Lips, tongue, or face are visibly swelling
- An EpiPen has been used (still need ER even if symptoms improve)
- Symptoms are spreading rapidly or worsening
- There is severe vomiting or persistent abdominal cramping with other symptoms
- The person has a known severe allergy and was exposed to that trigger
Why 911: paramedics carry epinephrine, oxygen, and IV fluids, and can begin treatment immediately. They also alert the ER so we’re ready when you arrive.
It May Be Safe to Walk In or Be Driven If:
- Symptoms are limited to skin (mild hives or rash) without facial or throat swelling
- Breathing is completely normal
- There is no dizziness, weakness, or low blood pressure feel
- Symptoms are not spreading or worsening
- You have someone else to drive — never drive yourself when symptomatic
If you are unsure, treat it as severe and call 911. Allergic reactions can change quickly.
How ER of Watauga Diagnoses an Allergic Reaction
Severe allergic reactions are usually diagnosed clinically — meaning the doctor recognizes the pattern of symptoms and starts treatment immediately, before any tests come back. Once you’re stable, additional testing helps identify the cause and prevent recurrence.
Our diagnostic process includes:
- Rapid clinical assessment — checking airway, breathing, circulation, skin, and mental status within seconds of arrival
- Vital sign monitoring — continuous tracking of blood pressure, oxygen, heart rate, and breathing
- Trigger history — what you ate, touched, were stung by, or took before symptoms began
- Blood tests (tryptase, CBC) — when needed, our full-service laboratory can confirm anaphylaxis and rule out other causes.
- EKG — for patients with chest pain, irregular pulse, or cardiac symptoms during the reaction, our EKG suite gives immediate results.
- Pulse oximetry and respiratory monitoring — detecting oxygen drops or wheezing early
- Imaging — rarely needed for allergic reactions, but available on-site if there are complications like swelling that may compromise the airway
Because every test is performed in-house, treatment never has to wait.
Allergic Reaction Treatment Options at Our ER

Treatment depends on severity. For severe reactions, we start aggressive treatment within seconds of arrival; for milder ones, we focus on symptom relief and prevention.
Treatments we provide on-site:
- Intramuscular epinephrine — first-line treatment for anaphylaxis, given immediately. Additional doses every 5–15 minutes if needed.
- IV fluids — to support blood pressure and combat shock, delivered through our IV fluids and antibiotics service.
- Oxygen therapy — to support breathing during airway swelling or low oxygen
- Antihistamines (H1 and H2 blockers) — to control hives, itching, and GI symptoms
- Corticosteroids — to reduce inflammation and lower the risk of biphasic (delayed) reactions
- Bronchodilators (albuterol) — for wheezing or asthma-like symptoms
- Vasopressors — for severe drops in blood pressure not responding to fluids and epinephrine
- Airway management — including intubation if there is severe throat swelling
- Observation period — for severe reactions, we monitor for 4–6 hours (sometimes longer) to watch for biphasic reactions
Most patients are stabilized within minutes and discharged the same visit, with prescriptions, EpiPen instructions, and a clear plan for follow-up with an allergist.
After the ER: Discharge and Prevention
Recovering from an allergic emergency doesn’t end when you leave the ER. Preventing the next one matters just as much.
Standard discharge instructions:
- Get and carry two EpiPens (one is sometimes not enough)
- Take antihistamines and corticosteroids exactly as prescribed for the next several days
- Watch for biphasic reactions for 24–72 hours and return to the ER if symptoms recur
- Avoid the suspected trigger until you’ve been evaluated by an allergist
- See an allergist for skin or blood testing to confirm the trigger
- Update your medical alert bracelet, school nurse, employer, and emergency contacts
- Make sure family and close friends know how to recognize symptoms and use an EpiPen
If you’ve had a severe reaction once, the next one can be even more severe. Treat your prevention plan with the same urgency you treated the emergency.
Why Choose ER of Watauga for Allergic Emergencies
With anaphylaxis, the speed of treatment is the single biggest factor in outcome. A hospital ER may have you wait while we already have you stabilized.
What sets us apart:
- Open 24/7, 365 days a year — including nights, weekends, and holidays
- Minutes-not-hours wait time — most patients are seen within minutes of arrival
- Full emergency capability on-site — IV access, epinephrine, oxygen, lab, EKG, all under one roof
- Board-certified emergency physicians — trained in critical airway and anaphylaxis management
- Dedicated pediatric emergency care — children are seen and treated with size-appropriate dosing and child-friendly care
- 9-star Google rating across 950+ verified patient reviews
- No surprise billing — transparent costs, in-network with most major insurance
For more on how a freestanding ER differs from urgent care, see our guide on Freestanding ER vs Urgent Care — urgent cares are not equipped to manage anaphylaxis.
Cost, Insurance, and Billing
Severe allergic reactions are medical emergencies. Federal law (EMTALA) requires us to evaluate and stabilize you regardless of ability to pay. Beyond that, we work hard to keep your costs predictable.
- Most major commercial insurance plans accepted (see our insurance coverage page)
- No surprise billing — you’ll never receive an unexpected bill
- Flexible payment plans through our Sunbit Payment Plan
If you are uncertain about coverage, our team will walk you through your options before non-emergency portions of treatment begin.
How to Reach ER of Watauga

We’re a walk-in 24-hour emergency room. No appointments needed.
Address: 5401 Basswood Blvd, Fort Worth, TX 76137
Phone: (817) 945-5500
Hours: Open 24 hours, 7 days a week
Service Area: Watauga, Fort Worth, North Richland Hills, Haltom City, Keller, Hurst, Bedford, Saginaw, and surrounding cities
If symptoms are severe, call 911 first. If symptoms are mild and you’re being driven, call ahead so our team is ready when you arrive.
Frequently Asked Questions About Allergic Reaction Emergencies
How fast can an allergic reaction become life-threatening?
Anaphylaxis can progress from mild symptoms to airway closure or shock in 10 to 15 minutes — sometimes faster, especially with insect stings or IV medications. The faster symptoms appear after exposure, the more dangerous the reaction is likely to be. When in doubt, treat as anaphylaxis and call 911.
Can Benadryl alone treat anaphylaxis?
No. Antihistamines like Benadryl can help with hives and itching, but they do not stop anaphylaxis. Only epinephrine reverses the airway swelling and blood pressure drop that make anaphylaxis fatal. If you suspect anaphylaxis, use an EpiPen first, then call 911 — antihistamines are an add-on treatment, not a substitute.
Do I really need to go to the ER if my EpiPen worked?
Yes. Up to 20% of anaphylaxis patients have a biphasic reaction — symptoms return hours after the initial event. Epinephrine also wears off in 15–20 minutes, while the allergic reaction can last much longer. Always go to the ER after using an EpiPen, even if you feel completely better.
How long will I need to stay at the ER after a severe reaction?
Most severe allergic reaction patients are observed for 4 to 6 hours after symptoms resolve to watch for biphasic reactions. Some cases — especially those needing multiple epinephrine doses — may need overnight monitoring. We’ll explain your specific timeline based on your symptoms and response to treatment.
Can I have an allergic reaction to something I’ve eaten safely before?
Yes. Allergies can develop at any age, and tolerance can change over time. People can become allergic to foods or medications they’ve used safely for years, sometimes after just one reaction. If you experience a new allergic reaction, take it seriously — even if you’ve eaten or taken the substance before.
What should I do while waiting for the ambulance?
Have the person lie flat with legs slightly raised (unless they have trouble breathing — then sit them upright). If they vomit or are unconscious, place them on their side. If they have an EpiPen and haven’t used it yet, use it. Loosen tight clothing. Do not give food, drink, or oral medication — they may need anesthesia or have airway swelling. Stay with them until help arrives.
Don’t Wait — Allergic Reactions Can Escalate in Minutes
Time matters more in allergic emergencies than almost any other condition. If you or someone you love is having a severe reaction, use an EpiPen if available, call 911, and come straight to the ER. For milder reactions that aren’t improving, walk in any time — we’re ready 24/7.
Open 24/7. Anaphylaxis-ready. No appointment needed.
|
🚨 Severe symptoms? Use EpiPen + call 911. 📞 ER of Watauga: (817) 945-5500 📍 5401 Basswood Blvd, Fort Worth, TX 76137 🕐 Open 24/7 |
ER of Watauga — fast, expert allergic reaction emergency care for the families of Watauga, Fort Worth, and surrounding North Texas communities.